November 2021, Kajiado County, Kenya – Walk into Enchula Resort Hotel in Kajiado County and you find a hive of activity. Small groups of masked health providers cluster round hospital beds where dummy babies are being ‘delivered’ from an actress (one of the nurses). Whiteboards are filled with penned instructions; ‘how to initiate a partograph’, ‘five steps to conflict resolution’. The room hums with terminology that would sound foreign to the untrained ear; ‘vigorous births’, ‘shoulder dystocia’, ‘breech delivery’.
The scene typifies our centralized EmONC Mentorship training, a series of week-long intensive course aimed at increasing and sustaining provider skills in basic and emergency obstetric and newborn care (EmONC), and empowering them to continue mentorship support at their respective facilities. Our innovative ‘training of trainers’ model – which is deployed and actively used across thirteen Kenyan counties – encourages counties and sub-counties to take ownership of improvements to maternal and newborn health care quality, and sustains a constant cycle of skills-building within facilities – all meaning mums and babies are served by competent, respectful maternity nurses.
Testing the effectiveness of MENTORS in select Kenyan counties
The three centralized trainings – taking place in Kisi, Meru, and Kajiado – feed into a wider randomized control trial Jacaranda is conducting to determine the effectiveness of our package of complementary solutions on patient and provider outcomes in Kenya’s public facilities. Results from the trial will, in time, be shared with Directors of Health, Department of Family Health, county leadership, as well as facilities through technical working groups, helping us pave the way to national scale-up.

The week starts by going back to basics. Understanding mentorship as coming in many guises, our lead mentors begin with some simple questions; ‘what makes a good mentor?’, ‘what role do they play in maternal health?’, ‘what kind of barriers exist to mentorship?’, and ‘how does mentorship actually benefit providers in facilities?’. Openly discussing the basic principles of effective mentorship helps build accountability; mentors are encouraged to see the value and potential impact in their new roles. Reinforcing this accountability, the week is bookended by a final goal-setting session where mentors are asked “how much are you willing to put in?”, and they openly commit to routine monthly mentorship.
Our EmONC curriculum is designed to not only build competence, but also confidence. Throughout the week, mentors learn the principles of respectful care, how to develop and facilitate Continuous Medical Education (CME), and a roster of new communications skills – both when talking to the mums they care for, as well as reporting on their condition following a ‘Situation, Background, Assessment, Recommendation’ stepwise approach.
‘As the ones on the ground, the mentors are already experts in the problems in their facilities. They are equipped with the skills to address these challenges – and empower others to address them – in a way that is evidence-based and has had proven success in the past.’
– Teresiah Gatitu, Lead Mentor, Jacaranda Health
Real-life simulation to build practical skills to counter emergencies
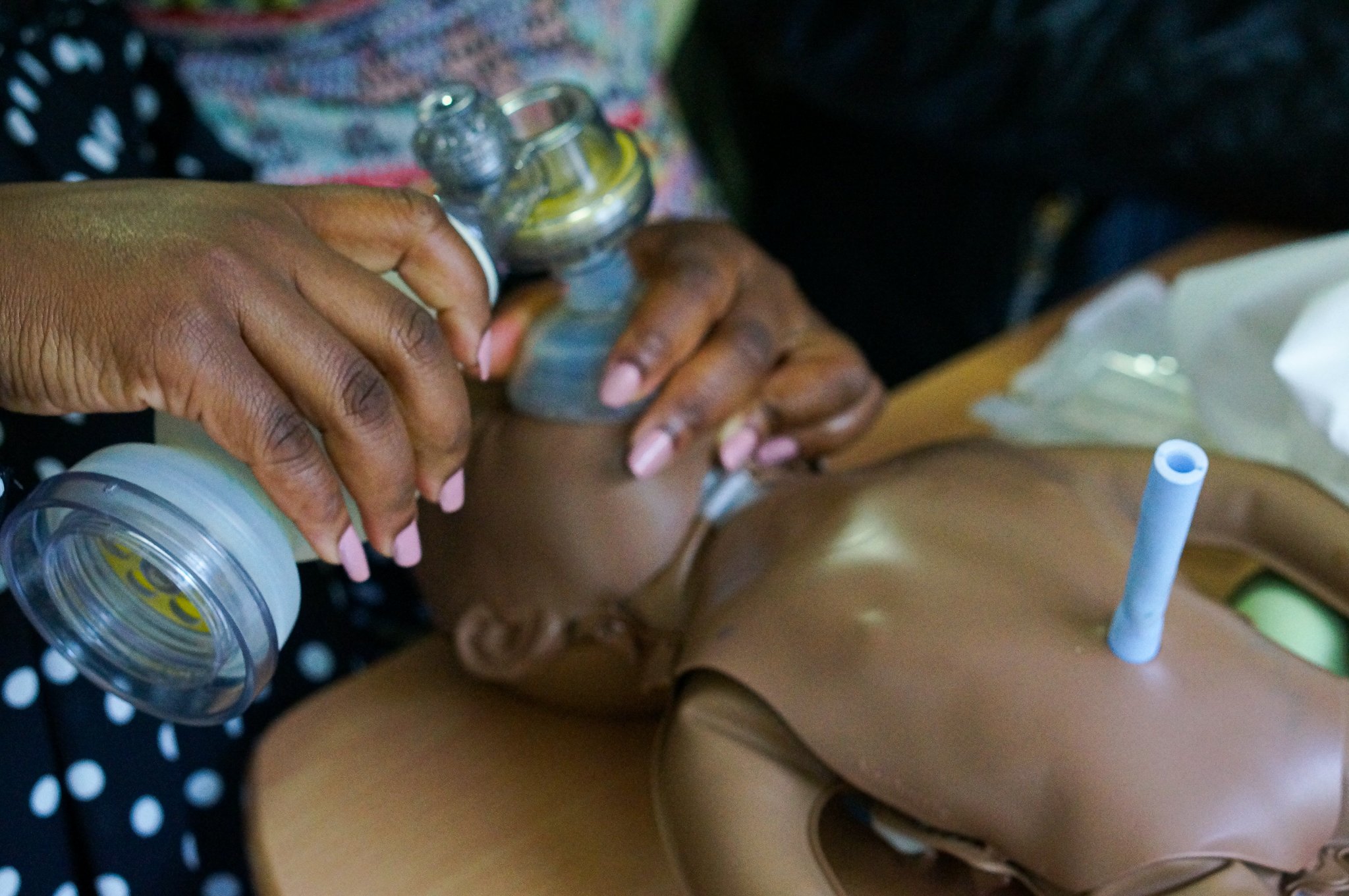
Simulation is a critical part of the EmONC training package, plunging providers into ‘real-life’ emergency scenarios to test not only their clinical competence, but also ability to communicate, lead, and problem solve in high pressure environments. Today, mentors are performing an obstetric simulation. The scenario depicts a woman with severe postpartum hemorrhage (excessive bleeding after delivery), and showing signs of shock.
One mentor takes the role of the mother in distress, the others gather in small groups as they methodically apply their learnings to the situation at hand; first, wash hands thoroughly with soap and water, second, establish an IV line using normal saline, then, inject four grams of magnesium sulphate with sterile water or saline over 5 – 20 minutes’. The drill is followed by a simulation debrief where providers and health coordinators discuss how the provider administering the drugs performed; what could have been done differently, and what parallels it shares with real life situations in their own facilities.
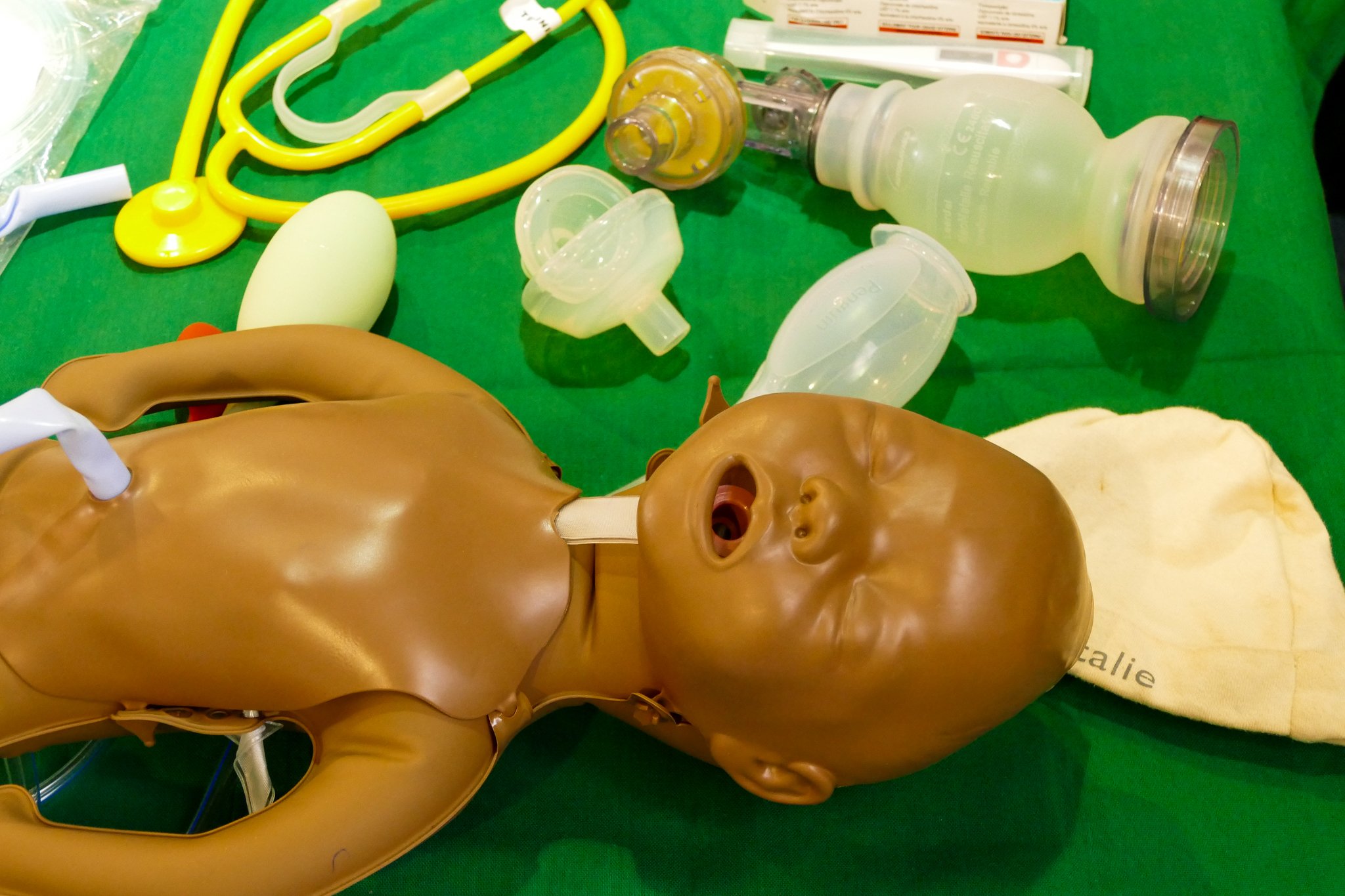
Later, mentors team up with new counterparts to simulate an emergency response to a woman showing signs of preeclampsia, seizures that occur during a woman’s pregnancy. Drills are brought to life through ‘JESCO packs’ (Jacaranda Enhancing Safe Care in Obstetrics). Just as you’d find in a delivery room, waterproof knickers and liners are on-hand for vaginal leakage after birth. Mentors help ‘deliver’ and care for baby Natalie, a realistic newborn doll, and rubber bands are used to mimic the insertion of a cannula, a thin plastic tube inserted into a vein supplying vital medication to mums during and after delivery. The pack even includes food coloring to create a blood-like fluid.
What does this mean for skills and knowledge in facilities?
This practical application of classroom learning helps test and reinforce the various aspects of emergency response for mentors, empowering them to return and train up providers in their respective facilities, as well as seeing firsthand the power of simulation and its use as a powerful training model. All mentors are provided an EmONC booklet, offering easy-to-read step-by-step information on the four drills; eclampsia, normal birth of vigorous baby, normal birth of non-vigorous with severe postpartum hemorrhage and signs of shock, and preterm labor and non-vigorous baby.
The program is deliberately inclusive of a variety of health system levels, which helps ensure improvements in care quality are both enforced and maintained within facilities. County and subcounty reproductive health coordinators (RHCs) learn alongside health providers from twenty facilities including clinicians, maternity nurses, and doctors. This diversity – of disciplines, levels, facilities, and even counties – is instrumental in the sharing of ideas, resources and learnings around emergency care, as well as an opportunity for Jacaranda to learn more about common bottlenecks to care provision across Kenya.