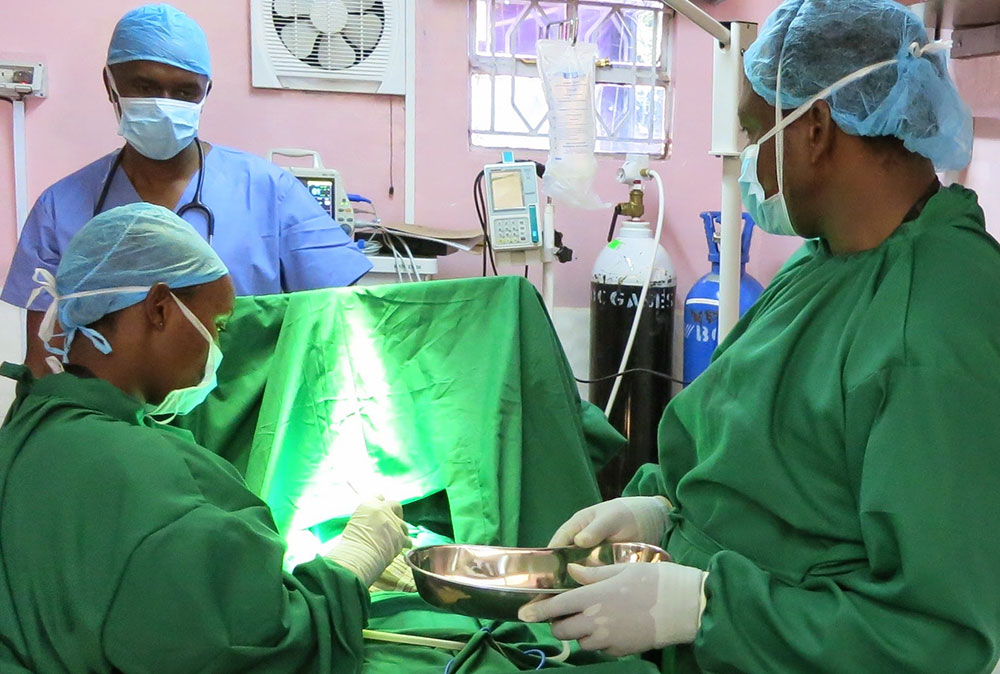
A mother is moaning in pain as she feels the urge to push. A nurse rushes to check her blood pressure. Another nurse is talking calmly to the mother and her birth companion, while supporting them through the entire process, step by step, until finally, the baby has been delivered. She takes a deep breath, but then the nurse notices a shock: heavy bleeding. Postpartum hemorrhage, one of the top causes of maternal death worldwide. The nurse, determined to keep her composure, gains control of the situation and begins the process she has practiced over and over for this scenario – massage the uterus, check for the cause, administer oxytocin. The mother lives.
Jacaranda’s Nurse Mentorship Program
For the above scenario to end well in a public hospital, providers need appropriate and repeated training – not just classroom training, but a system for regular drills and continued mentorship. Jacaranda’s team of Nurse Mentors work with public facility nurses to sustainably improve emergency obstetric and newborn care (EmONC). Jacaranda’s approach to clinical innovation is to borrow evidence-based global best practices and then work with government partners, nurses, and end users to co-design and adapt them to be suitable and sustainable in the public health system. In this case, we draw on approaches from experts in the field of obstetric and neonatal health, including PRONTO International for low-resource, high-fidelity simulation drills, Helping Babies Breathe for neonatal resuscitation, the WHO and the Kenya Ministry of Health for medical education lectures and guidelines, and Still-A-Mum for birth crisis education for providers. Our mentorship program has significantly improved nurse performance, and an encouraging indicator of success is that government partners are increasingly contributing to the costs of running the program.
The need for a Nurse Mentor Training Center (NMTC)
Jacaranda is currently working with five county partners across 45 public facilities, and we have seen rapidly growing demand from other counties to join the program. As the program expands, we need to build a pipeline for deploying nurse mentors across the country. Although the nurse mentorship program takes place in the public hospitals themselves – the contexts where emergencies actually occur — we needed a dedicated training center to building the capacity of the mentors themselves.
Technical Lead Dr. Sarah Little had a clear vision for the NMTC: a space that is inviting, encourages learning-by-doing, helps people generate ideas and inspires them while they’re learning and working. As we looked to contextualize global best practices we also compared notes with other training programs like the Center for Medical Simulation at Kijabe Hospital. The staff at Kijabe’s center shared their experiences and best practices, which helped inform our approach.
Building the NMTC
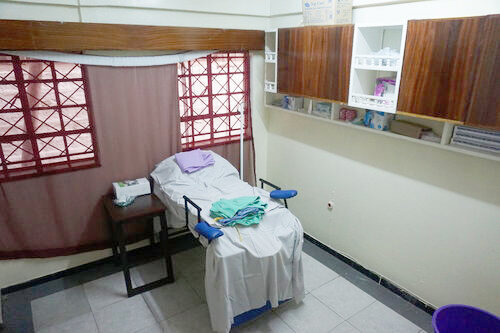
To keep costs as low as possible, we identified local sources for many components of the training process – medical kits, fake blood, standardized patient outfits. By engaging with local suppliers, Operations Lead Onana Omwodo was able to reduce the cost of these components by 75%. Finding local suppliers is critical for making these programs sustainable over time and demonstrates to our county partners that they can do it themselves.
To enhance the learning process, mentors and mentees can analyze the actions taken during simulation drills via CCTV camera footage on a TV screen, while sitting in a training room next door to the simulation taking place. “This allows people outside the scenario to observe while maintaining the fidelity of the simulation in the room. Then everyone involved can debrief and discuss what happened from the replay, all in a safe environment,” said Rachel Jones, Senior Programs Manager.
Open for business!

In June, after three months of hard work to launch the NMTC, our first cohort of mentor trainees walked into a facility that combines local materials with professional equipment, a delivery simulation room and adjacent classroom – all interconnected in a colorful, creatively-designed space.
For apprentice Nurse Mentor Janet Achieng, the training at the NMTC has paid off — “We have learned how to prepare for simulations and have run some of them ourselves. It’s been fun and during the last drills we were excited and ready,” said Janet, who will be embedded in public hospitals. “I really can’t wait to be a Nurse Mentor.”
Our goal is for Jacaranda’s NMTC to become a regional hub for mentor training, and a key step in our process of scaling our mentorship program across the country.